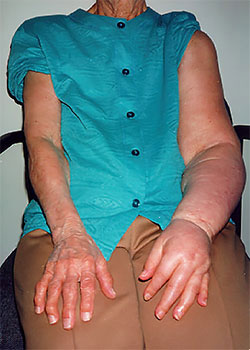
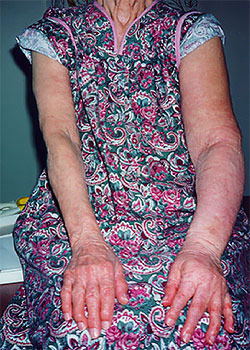
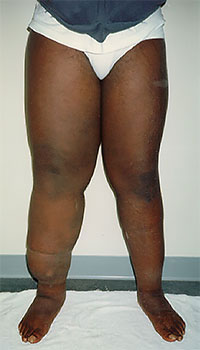
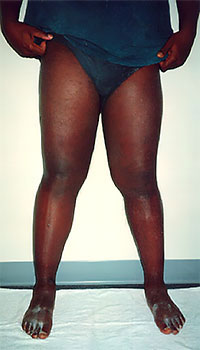
BACKGROUND
Lymphedema is a swelling of a body part usually occurring in the extremities. It can also occur in the face, neck, abdomen, or genitals. Lymphedema is the result of the abnormal accumulation of protein-rich edema fluid in the affected area. Remarkably, even though it afflicts approximately 1% of the U.S. population (nearly 3 million Americans), there is a shortage of lymphedema information, and the problems it creates are poorly understood in the medical community. Lymphedema is classified as either primary or secondary. Primary lymphedema is the result of lymphatic dysplasia. It may be present at birth but more often develops later in life without obvious cause. Secondary lymphedema is much more common and is the result of surgery or is a side effect of radiation therapy for cancer. Secondary forms may also occur after injury, scarring, trauma, or infection of the lymphatic system. Lymphedema has important pathological and clinical consequences. In stage I lymphedema, the swelling consists of protein-rich fluid and may be temporarily reduced by simple elevation of the limb. If it remains untreated, however, the lymphedema causes a progressive hardening of the affected tissues which is the result of a proliferation of connective tissue, adipose tissue, and scarring (stage II lymphedema). Stage III lymphedema is characterized by a tremendous increase in volume, hardening of the dermal tissues, hyperkeratosis, and papillomas of the skin. Infections such a cellulitis, erysipelas, and lymphangitis frequently develop in individuals suffering from lymphedema. Infections are most common in stage II and III lymphedema with each infection contributing to a worsening of the condition making frequent hospitalizations necessary. Lymphedema treatment options offered in the United States include surgery, medication, pneumatic compression pump therapy, Manual Lymph Drainage (MLD), and Complete Decongestive Therapy (CDT).
STAGES OF LYMPHEDEMA
LATENCY STAGE
- • lymphatic transport capacity is reduced •
- • no visible/palpable edema •
- • subjective complaints are possible •
STAGE I
(Reversible Lymphedema)
- • accumulation of protein-rich edema fluid •
- • pitting edema •
- • reducible with elevation (no fibrosis) •
STAGE II
(Spontaneously Irreversible Lymphedema)
- • accumulation of protein-rich edema fluid •
- • pitting becomes progressively more difficult •
- • connective tissue proliferation (fibrosis) •
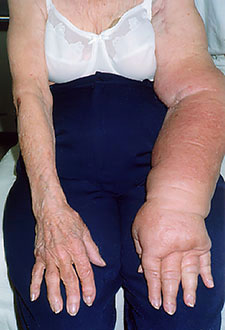
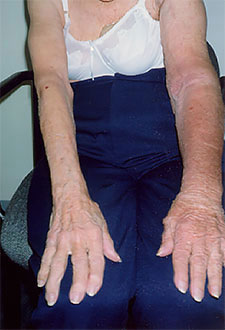
STAGE III
(Lymphostatic Elephantiasis)
- • accumulation of protein-rich edema fluid •
- • non-pitting •
- • fibrosis and sclerosis (severe induration) •
- • skin changes (papillomas, hyperkeratosis, etc.) •
MANUAL LYMPH DRAINAGE (MLD)
MLD, a gentle manual lymphatic therapy technique, is a potent way to activate the lymphatic system, especially when the transport capacity of the lymph vessel is reduced because of prior surgery and/or radiation therapy. However, if carried out as an isolated treatment for lymphedema, the results are very temporary and lasting evacuation of lymph fluid from a congested limb is not possible. Many MLD practitioners have been trained only in basic MLD and are not qualified to treat lymphedema at all. However, MLD alone may be used with much success in many conditions unrelated to lymphedema.
COMPLETE DECONGESTIVE THERAPY (CDT)
CDT is a combination of MLD, bandaging of the affected areas, remedial exercises, and skin and nail care. CDT is divided into a two-phase program that initially involves an intensive treatment phase and is then followed by a maintenance program continued by the patient at home. Carried out with great care and consistency by a certified lymphedema therapist, CDT is the treatment of choice for chronic extremity lymphedema. Even in advanced lymphedema, CDT achieves excellent results with no side effects. Because CDT is labor intensive, time-consuming, and requires patient compliance, many patients have difficulty committing to the program at first. However, because the results of CDT are always superior to those achieved with all other treatments, increasing numbers of patients are undergoing CDT treatment and are consequently able to maintain the reduction of their limbs through diligent participation in a home maintenance program. Because CDT is fairly new in the United States, staff training and treatment standards vary from clinic to clinic. For a lymphedema therapist to be fully competent in treating lymphedema using CDT, it is vital that the CDT training consist of the four components of CDT: (1) basic and advanced MLD, (2) lymphedema bandaging, (3) remedial exercises, (4) skin and nail care. The therapist must also have a complete understanding of the anatomy, physiology, and pathophysiology of the lymphatic system, the treatment of primary and secondary lymphedema, the indications and contraindications of CDT, and the proper measuring techniques for lymphedema support garments. Furthermore, lymphedema therapy should not begin unless the patient has been examined and diagnosed by a board-certified physician who understands lymphedema and its complications. Once the diagnosis of lymphedema has been confirmed and treatment has begun, the progress must be monitored by the physician. Whereas the clinical diagnosis of lymphedema can most often be established without invasive testing, and electrocardiogram before the treatment begins and during the course of treatment is sometimes necessary to ensure safe treatment for each patient. Lymphangioscintigraphy (LAS), CT scans, and MRIs are also recommended for lymphedema patients before starting CDT. The physician will be able to decide and inform the patient about the necessity of such procedures at the time of consultation. Because of the complications associated with lymphedema, the involvement and supervision of a qualified physician is essential for safe and effective lymphedema therapy.
SURGERY
Surgical procedures are sometimes suggested to a lymphedema patient. Numerous operational procedures have been devised and thousands of operations have been carried out over the past century. None of the surgical techniques has been shown to give consistent or dependable results. In addition, any surgery performed on a lymphedematous (swollen) extremity may further reduce the transport capacity of an already-incapacitated lymphatic system.
MEDICATIONS
Diuretics, while often prescribed, usually make the lymphedema worse. Diuretics are able to draw off the water content of the edema while the protein molecules remain in the tissue spaces. These proteins continue to draw water to the edematous areas as soon as the diuretic loses its effectiveness. These accumulated proteins also lead to a higher concentration of proteins in the edema fluid and cause the tissues to become even more fibrotic and indurated. Benzopyrones for lymphedema have been tried for many years, primarily in other countries. Their therapeutic effect as it relates to lymphedema continues to be debated. Furthermore, the product lacks FDA approval. Some patients who have used the drug here in the United States have discontinued its use after having experienced adverse side effects.
PUMP THERAPY
The pneumatic compression pump is a mechanical device that "milks" the lymph fluid out of the swollen extremity. The problems with pneumatic pumps are numerous and any results achieved are usually very temporary. Pump therapy, for instance, disregards the fact that the ipsilateral trunk quadrant is also more or less congested or lymphedematous. Hence, lymph fluid that is pumped into the trunk quadrant adjacent to the lymphedematous extremity will create congestion, connective and scar tissue, and induration (hardening) at the root of the extremity, namely the hip and buttock areas in lower extremity lymphedema and the shoulder, chest, and back areas in upper extremity lymphedema. This lymphedema will continue to worsen in spite of vigorous pumping. In lower extremity lymphedema, extensive pumping may cause genital lymphedema, which will not only create more physical difficulties but also immense psychological problems for the patient. In addition, pumps do nothing to eliminate scar and connective tissue (lymphatic fibrosis) which always exist in stage II and III lymphedema. In most cases, lymphedema recurs the moment the patient stops using the compression pump.
Pump therapy is still offered in many treatment centers. Some clinics use pumps because of the financial advantages achieved through facilitated insurance reimbursement. In addition, it is quite easy to place a patient on a pump without the attention of qualified or experienced personnel. Some clinics may also use pumps because they simply do no have trained lymphedema therapists on staff.